An evolving guide to the diseases in the game and how they affect the animals.
But, first and foremost, all info provided is merely to satisfy gamer curiosity. I am neither a vet, nor a doctor. What do I know?! But, hey, have fun!
 Influenza A virus is a zoonotic infection with a natural reservoir almost entirely in birds. Several domestic species have been infected, including cats, dogs, ferrets, pigs, and birds. But, it also infects seals as well. The Influenza A has adapted itself well to one species which then carries it to other animals that have no immunity or resistance.
Influenza A virus is a zoonotic infection with a natural reservoir almost entirely in birds. Several domestic species have been infected, including cats, dogs, ferrets, pigs, and birds. But, it also infects seals as well. The Influenza A has adapted itself well to one species which then carries it to other animals that have no immunity or resistance.
People who do not regularly come into contact with birds are not at high risk for contracting avian influenza. Those at high risk include poultry farm workers, animal control workers, wildlife biologists, and ornithologists who handle live birds. It is most often spread by contact between infected and healthy birds, though it can also be spread indirectly through contaminated equipment. The virus is found in secretions from the nostrils, mouth, and eyes of infected birds as well as their droppings. HPAI infection is spread to people often through direct contact with infected poultry, such as during slaughter or plucking.
Though the virus can spread through airborne secretions, the disease itself is not an airborne disease. Highly pathogenic strains spread quickly among flocks and can destroy a flock within 28 hours; the less pathogenic strains may affect egg production but are much less deadly.
Although it is possible for humans to contract the avian influenza virus from birds, human-to-human contact is much more difficult without prolonged contact. However, public health officials are concerned that strains of avian flu may mutate to become easily transmissible between humans. Some strains of avian influenza are present in the intestinal tract of large numbers of shore birds and water birds, but these strains rarely cause human infection.
Five man-made ecosystems have contributed to modern avian influenza virus ecology: integrated indoor commercial poultry, range-raised commercial poultry, live poultry markets, backyard and hobby flocks, and bird collection and trading systems including cockfighting. Indoor commercial poultry has had the largest impact on the spread of HPAI, with the increase in HPAI outbreaks largely the result of increased commercial production since the 1990s.
The Cheetahs in my habitat should have no worries, since they are in a dedicated environment. (From an in-game screenshot.)
 The only info I have found here calls it “Canine Respiratory Bordetellosis…an Evolving Pathogen.”
The only info I have found here calls it “Canine Respiratory Bordetellosis…an Evolving Pathogen.”Not much to go on there, except that it is a doggy disease. (My screenshot from in-game features a battle royale between an Arctic Wolf female and a male Timberwolf.)
 Botulism affects many species of both vertebrates and invertebrate animals: including birds, ducks, rats, mice, chicken, frogs, toads, and goldfish. Up to 100,000 birds die of botulism annually. The disease is commonly called “limberneck.” The Western USA and Canada has a variety called “western duck sickness”.
Botulism affects many species of both vertebrates and invertebrate animals: including birds, ducks, rats, mice, chicken, frogs, toads, and goldfish. Up to 100,000 birds die of botulism annually. The disease is commonly called “limberneck.” The Western USA and Canada has a variety called “western duck sickness”.
Botulism also affects commercially raised poultry. In chickens, the mortality rate varies from a few birds to 40% of the flock. Though it is uncommon in domestic mammals, it can kill cattle and horses in epidemics. Pigs seem more resistant. Diarrhea is one of the common symptoms. (My screenshot of Peafowls from in-game.)
 The food poisoning/ diarrhea disease is usually caused by C. jejuni, a spiral and comma shaped bacterium normally found in cattle, swine, and birds, but the illness can also be caused by C. coli (also found in cattle, swine, and birds), C. upsaliensis (found in cats and dogs) and C. lari (present in seabirds in particular).
The food poisoning/ diarrhea disease is usually caused by C. jejuni, a spiral and comma shaped bacterium normally found in cattle, swine, and birds, but the illness can also be caused by C. coli (also found in cattle, swine, and birds), C. upsaliensis (found in cats and dogs) and C. lari (present in seabirds in particular).
IMHO animals tend to get this if the water is not clean in my zoo. (The screenshot features some of the bird species in the outdoor Aviary in my Varirata Zoo.
 Sometimes called hardpad disease, this is a viral disease that affects many animal families, including domestic and wild species of dogs, coyotes, foxes, pandas, wolves, ferrets, skunks, raccoons, and large cats, as well as pinnipeds (seals), some primates, and a variety of other species. Animals in the cat family were long believed to be resistant to canine distemper, until some researchers reported the prevalence of symptom-less CDV infection in large felines, usually through close housing with dogs or possibly blood transfusion from infected cats.
Sometimes called hardpad disease, this is a viral disease that affects many animal families, including domestic and wild species of dogs, coyotes, foxes, pandas, wolves, ferrets, skunks, raccoons, and large cats, as well as pinnipeds (seals), some primates, and a variety of other species. Animals in the cat family were long believed to be resistant to canine distemper, until some researchers reported the prevalence of symptom-less CDV infection in large felines, usually through close housing with dogs or possibly blood transfusion from infected cats.
In canines, distemper affects several body systems, including the gastrointestinal and respiratory tracts and the spinal cord and brain, with common symptoms that include high fever, eye inflammation and eye/nose discharge, labored breathing and coughing, vomiting and diarrhea, loss of appetite and lethargy, and hardening of nose and footpads. The viral infection can be accompanied by secondary bacterial infections and can present eventual serious neurological symptoms.
Canine distemper is caused by the same family of viruses that causes measles, mumps, and bronchiolitis in humans. The disease is highly contagious via inhalation. Morbidity and mortality may vary greatly among animal species, with up to 100% mortality in unvaccinated populations of ferrets. In domestic dogs, while the acute generalized form of distemper has a high mortality rate, disease duration and severity depends mainly on the animal’s age and immune status and virulence of the infecting strain of the virus. Despite extensive vaccination in many regions, it remains a major disease of dogs, and was the leading cause of infectious disease death in dogs, prior to a vaccine becoming available. (The Timberwolves mating in my screenshot get the ‘Loving Cup award.’)
The game has Common Warthogs, but since they are so ugly, I rarely photograph them. 🙂 I feel the same about the Tapirs and Aardvarks.
 Today, the virus is found in Europe, mainly in the UK. Human cases are very rare and most often contracted from domestic cats. Human infections usually remain localized and self-limiting, but can become fatal in immunosuppressed patients. The virus is not commonly found in cattle; the reservoir hosts for the virus are woodland rodents, particularly voles. Domestic cats contract the virus from these rodents. Symptoms in cats include lesions on the face, neck, forelimbs, and paws, and, less commonly, upper respiratory tract infections. Symptoms of infection with cowpox virus in humans are localized, pustular lesions generally found on the hands and limited to the site of introduction. The incubation period is 9 to 10 days. The virus is most prevalent in late summer and autumn. Cowpox is an infectious disease caused by the cowpox virus. The virus is zoonotic, meaning that it is transferable between species, such as from animal to human.
Today, the virus is found in Europe, mainly in the UK. Human cases are very rare and most often contracted from domestic cats. Human infections usually remain localized and self-limiting, but can become fatal in immunosuppressed patients. The virus is not commonly found in cattle; the reservoir hosts for the virus are woodland rodents, particularly voles. Domestic cats contract the virus from these rodents. Symptoms in cats include lesions on the face, neck, forelimbs, and paws, and, less commonly, upper respiratory tract infections. Symptoms of infection with cowpox virus in humans are localized, pustular lesions generally found on the hands and limited to the site of introduction. The incubation period is 9 to 10 days. The virus is most prevalent in late summer and autumn. Cowpox is an infectious disease caused by the cowpox virus. The virus is zoonotic, meaning that it is transferable between species, such as from animal to human.
The transferral of the disease was first observed in dairymaids who touched the udders of infected cows and consequently developed the signature pustules on their hands. Cowpox is more commonly found in animals other than bovines, such as rodents. Cowpox is similar to, but much milder than, the highly contagious and often deadly smallpox disease. Its close resemblance to the mild form of smallpox and the observation that dairy farmers were immune to smallpox inspired the first smallpox vaccine, created and administered by English physician Edward Jenner.
The word “vaccination,” coined by Jenner in 1796, is derived from the Latin root vaccinus, meaning of or from the cow. The cowpox vaccinations and later incarnations proved so successful that in 1980, the World Health Organization announced that smallpox was the first disease to be eradicated by vaccination efforts worldwide. Other orthopox viruses remain prevalent in certain communities and continue to infect humans, such as the cowpox virus (CPXV) in Europe, vaccinia in Brazil, and monkeypox virus in Central and West Africa.
(My screenshot here features an escaped and carefree West African Lioness.)
 Elephant endotheliotropic herpesviruses (EEHV) or Elephantid betaherpesvirus 1 (ElHV-1) is a type of herpes virus, which can cause a highly fatal hemorrhagic disease when transmitted to young Asian elephants. In African elephants, related forms of these viruses, which have been identified in wild populations, are generally benign, occasionally surfacing to cause small growths or lesions. However, some types of EEHV can cause a highly fatal disease in Asian elephants, which kills up to 80% of severely affected individuals.
Elephant endotheliotropic herpesviruses (EEHV) or Elephantid betaherpesvirus 1 (ElHV-1) is a type of herpes virus, which can cause a highly fatal hemorrhagic disease when transmitted to young Asian elephants. In African elephants, related forms of these viruses, which have been identified in wild populations, are generally benign, occasionally surfacing to cause small growths or lesions. However, some types of EEHV can cause a highly fatal disease in Asian elephants, which kills up to 80% of severely affected individuals.
The disease can be treated with the rapid application of antiviral drugs, but this has only been effective in around a third of cases. Those affected are mostly young animals born in captivity, though a small number of older wild-born adults held in zoos have died, and a number of cases caused by the same pathogenic type of EEHV have been identified in both orphan and wild calves in Asian elephant populations.
(My screenshot from in-game.)
 Feline infectious peritonitis (FIP) is the name given to an uncommon, but usually fatal, aberrant immune response to infection with feline coronavirus (FCoV.) FCoV is a virus of the gastrointestinal tract: most infections cause diarrhea, (or are symptomless) especially in kittens, who are weaned between 5 and 7 weeks of age. The mother’s milk gives them anitbodies before that. The virus is a mutation of feline enteric coronavirus (FECV). From the gut, the virus very briefly undergoes a systemic phase, returning to the gut, from where it is shed in the feces.
Feline infectious peritonitis (FIP) is the name given to an uncommon, but usually fatal, aberrant immune response to infection with feline coronavirus (FCoV.) FCoV is a virus of the gastrointestinal tract: most infections cause diarrhea, (or are symptomless) especially in kittens, who are weaned between 5 and 7 weeks of age. The mother’s milk gives them anitbodies before that. The virus is a mutation of feline enteric coronavirus (FECV). From the gut, the virus very briefly undergoes a systemic phase, returning to the gut, from where it is shed in the feces.
(The Cheetah Mother/ Daughter pair in my screenshot are enjoying swimming lessons.)
 Often called hoof-and-mouth disease (HMD) this is an infectious and sometimes fatal viral disease that affects cloven-hoofed animals, including domestic and wild bovids. The virus causes a high fever lasting two to six days, followed by blisters inside the mouth and on the feet that may rupture and cause lameness.
Often called hoof-and-mouth disease (HMD) this is an infectious and sometimes fatal viral disease that affects cloven-hoofed animals, including domestic and wild bovids. The virus causes a high fever lasting two to six days, followed by blisters inside the mouth and on the feet that may rupture and cause lameness.
But, do not worry. This is not the same disease as Hand, Foot, and Mouth disease which is a common children’s virus that only causes a rash and will not kill you.
(My screenshot features an American Bison capture.)

Signs of glanders include the formation of nodular lesions in the lungs and ulceration of the mucous membranes in the upper respiratory tract. The acute form results in coughing, fever, and the release of an infectious nasal discharge, followed by septicaemia and death within days. In the chronic form, nasal and subcutaneous nodules develop, eventually ulcerating; death can occur within months, while survivors act as carriers.
 Glanders was a major problem in warfare in the Middle Ages. Before the Battle of Blenheim in 1704, glanders may have afflicted and greatly diminished the horses of Marshal Tallard’s cavalry, helping the Duke of Marlborough win the battle. Interestingly, Glanders has been known since ancient times, and has been used in biological warfare by many countries in modern times, though it tends to lose virulence in the lab, making it difficult to weaponize.
Glanders was a major problem in warfare in the Middle Ages. Before the Battle of Blenheim in 1704, glanders may have afflicted and greatly diminished the horses of Marshal Tallard’s cavalry, helping the Duke of Marlborough win the battle. Interestingly, Glanders has been known since ancient times, and has been used in biological warfare by many countries in modern times, though it tends to lose virulence in the lab, making it difficult to weaponize.
Glanders is endemic in Africa, Asia, the Middle East, and Central and South America. It has been eradicated from North America, Australia, and most of Europe through surveillance and destruction of affected animals, and import restrictions.
Photo of Duke of Marlborough from Wikipedia article on the Battle of Blenheim
Many cases have few or no symptoms, especially in the young. The time between infection and symptoms, in those who develop them, is between two and six weeks. When symptoms occur, they typically last eight weeks and may include nausea, vomiting, diarrhea, jaundice, fever, and abdominal pain. Around 10–15% of people experience a recurrence of symptoms during the six months after the initial infection. Acute liver failure may rarely occur, with this being more common in the elderly. I am unsure of how it is exhibited in animals.
In humans it is usually spread by eating food or drinking water contaminated with infected feces. Shellfish which have not been sufficiently cooked are a relatively common source. It may also be spread through close contact with an infectious person. While children often do not have symptoms when infected, they are still able to infect others. After a single infection, a person is immune for the rest of his or her life. It is more common in regions of the world with poor sanitation and not enough safe water.
 Listeriosis is a bacterial disease that can affect all ruminants (mainly sheep and goats) as well as other animal species and humans. (My screenshot shows that predation is totally in the game. I put a Dall Sheep in the pen with a Timberwolf, but not for long.)
Listeriosis is a bacterial disease that can affect all ruminants (mainly sheep and goats) as well as other animal species and humans. (My screenshot shows that predation is totally in the game. I put a Dall Sheep in the pen with a Timberwolf, but not for long.)
It most commonly causes encephalitis, but is also capable of causing a blood infection and loss of babies to pregnant females. It is commonly seen in cooler climates. These bacteria can be found in the soil, food sources, and even the feces of healthy animals. Most commonly, this disease of sheep and goats is observed as a result of feeding moldy or spoiled hay or silage. But, it is also found in the environment. The bacteria are very hardy and are common in soil.
Symptoms of Listeriosis include depression, loss of appetite, fever, lack of coordination, salivation, facial paralysis, and circling. Disease is more common in animals 1 to 3 years of age than it is in older animals. The abortion form of Listerosis usually shows no other symptoms and can only be diagnosed by laboratory analysis. The onset of the encephalitic form is usually very fast and causes death in 24 to 48 hours after symptoms appear. Symptoms include circling in one direction, high fever, lack of appetite, red tissues around the eyes, usually with blindness, and depression. Affected animals may have a droopy ear, drooping eyelid, and saliva running from limp lips on one side of the face caused by a partial paralysis. When near death, the animal will lie down and may have convulsions. Recovery is rare.
 Monkeypox virus causes the disease in both humans and animals. It was first identified in 1958 as a pathogen of crab-eating macaque monkeys (Macaca fascicularis) being used as laboratory animals. The crab-eating macaque is often used for neurological experiments. Monkeypox virus is found mainly in tropical rainforest regions of Central and West Africa. Limited person-to-person spread of infection has been reported in disease-endemic areas in Africa.
Monkeypox virus causes the disease in both humans and animals. It was first identified in 1958 as a pathogen of crab-eating macaque monkeys (Macaca fascicularis) being used as laboratory animals. The crab-eating macaque is often used for neurological experiments. Monkeypox virus is found mainly in tropical rainforest regions of Central and West Africa. Limited person-to-person spread of infection has been reported in disease-endemic areas in Africa.
The primary route of infection is thought to be contact with the infected animals or their bodily fluids. Humans can be infected by an animal via a bite, or by direct contact with an infected animal’s bodily fluids. The virus can also spread from human to human, by respiratory (airborne) contact or by contact with an infected person’s bodily fluids. The incubation period is 10–14 days. Symptoms include swelling of lymph nodes, muscle pain, headache, and fever prior to the emergence of the rash. The rash is usually only present on the trunk, but may spread to the palms and soles of the feet in a centrifugal distribution. The initial macular lesions exhibit a papular, then vesicular and pustular appearance.
In addition to monkeys, reservoirs for the virus are found in Gambian pouched rats, dormice, and African squirrels. The use of these animals as food may be an important source of transmission to humans. (My screenshot is an in-game shot of a beautiful Mandrill.)
 MRSA refers to a group of bacteria that are genetically distinct from other forms of Staph. MRSA is responsible for several difficult-to-treat infections in humans. MRSA is any strain that has developed, through horizontal gene transfer and natural selection, multiple drug resistance to antibiotics. Antibiotic use in livestock increases the risk that MRSA will develop among the livestock; and in return be transmissible to humans. Generally, animals have no symptoms.
MRSA refers to a group of bacteria that are genetically distinct from other forms of Staph. MRSA is responsible for several difficult-to-treat infections in humans. MRSA is any strain that has developed, through horizontal gene transfer and natural selection, multiple drug resistance to antibiotics. Antibiotic use in livestock increases the risk that MRSA will develop among the livestock; and in return be transmissible to humans. Generally, animals have no symptoms.
We hear about MRSA often in the news because locker rooms, gyms, and related athletic facilities offer potential sites for MRSA contamination and infection. Athletes have been identified as a high-risk group.
I am unsure of the level to which animals can be infected by sharing connections between water sources that cross multiple habitats in-game. But, my pictured camels access only a section of the larger body of water in this desert oasis (my screenshot from in-game.) It is a safe bet that this may not be best practices. I am in the process of modifying the terrain in this franchise zoo, since disease was a problem at first.
Mycoplasma species are the smallest bacterial cells yet discovered, can survive without oxygen, and come in various shapes. For example, M. genitalium is flask-shaped, while M. pneumoniae is more elongated. Hundreds of mycoplasma species infect animals.
 Crocodiles serve as natural hosts for this genus of viruses. There is currently only one species in this genus, and that is the crocs. Diseases associated with the viruses include nodular skin lesions in young animals, a nonfatal dermatitis, a more severe disease characterized by ophthalmia, rhinitis resulting in asphyxia, and debilitating illness with stunting and high mortality. (My screenshot is from in-game.)
Crocodiles serve as natural hosts for this genus of viruses. There is currently only one species in this genus, and that is the crocs. Diseases associated with the viruses include nodular skin lesions in young animals, a nonfatal dermatitis, a more severe disease characterized by ophthalmia, rhinitis resulting in asphyxia, and debilitating illness with stunting and high mortality. (My screenshot is from in-game.)
The disease was first noted professionally in the late 1930’s in slaughterhouses. The pathogenic agent is found everywhere except New Zealand. The bacterium is extremely sustainable and virulent: a single organism is able to cause an infection. The common source of infection is inhalation of contaminated dust, contact with contaminated milk, meat, or wool, and particularly birthing products. Ticks can transfer the pathogenic agent to other animals. Transfer between humans seems extremely rare and has so far been described in very few cases.
There has been some investigation into use of the bacteria in biological warfare.
 Rotaviruses are the most common cause of diarrhoeal disease among infants and young children, as well as infecting zoo animals and livestock. Nearly every child in the world is infected with a rotavirus at least once by the age of five. Immunity develops with each infection, so subsequent infections are less severe; adults are rarely affected. The virus is transmitted by the faecal-oral route. (A good reason for Keepers to clean those habitats monthly!) It infects and damages the cells that line the small intestine and causes gastroenteritis (which is often called “stomach flu” despite having no relation to influenza). In addition to its impact on human health.
Rotaviruses are the most common cause of diarrhoeal disease among infants and young children, as well as infecting zoo animals and livestock. Nearly every child in the world is infected with a rotavirus at least once by the age of five. Immunity develops with each infection, so subsequent infections are less severe; adults are rarely affected. The virus is transmitted by the faecal-oral route. (A good reason for Keepers to clean those habitats monthly!) It infects and damages the cells that line the small intestine and causes gastroenteritis (which is often called “stomach flu” despite having no relation to influenza). In addition to its impact on human health.
Rotaviruses infect the young of many species of animals and they are a major cause of diarrhoea in wild and reared animals worldwide. As a pathogen of livestock, notably in young calves and piglets, rotaviruses cause economic loss to farmers because of costs of treatment associated with high morbidity and mortality rates. These rotaviruses are a potential reservoir for genetic exchange with human rotaviruses. There is evidence that animal rotaviruses can infect humans, either by direct transmission of the virus or by contributing one or several RNA segments to reassortants with human strains.
Since Rotaviruses are highly contageous, ‘an ounce of prevention is worth a pound of cure.’ Common treatments are often ineffective after infection. But, vaccination helps prevent the spread of the diseases.
 This is an infection caused by bacteria/ food poisoning. The most common symptoms are diarrhea, fever, abdominal cramps, and vomiting. Symptoms typically occur between 12 hours and 36 hours after exposure, and last from two to seven days. Occasionally more significant disease can result in dehydration. The old, young, and others with a weakened immune system are more likely to develop severe disease. Specific types of Salmonella can result in typhoid fever or paratyphoid fever.
This is an infection caused by bacteria/ food poisoning. The most common symptoms are diarrhea, fever, abdominal cramps, and vomiting. Symptoms typically occur between 12 hours and 36 hours after exposure, and last from two to seven days. Occasionally more significant disease can result in dehydration. The old, young, and others with a weakened immune system are more likely to develop severe disease. Specific types of Salmonella can result in typhoid fever or paratyphoid fever.
Infection is usually spread by eating contaminated meat, eggs, or milk. Other foods may spread the disease if they have come into contact with manure. It is a disease which infects humans, as well as one which can be carried and spread by a number of pets; including cats, dogs, and reptiles.
Efforts to prevent the disease include the proper washing, preparation, and cooking of food. Mild disease typically does not require specific treatment. More significant cases may require treatment of electrolyte problems and intravenous fluid replacement. In those at high risk or in whom the disease has spread outside the intestines, antibiotics are recommended.
Salmonellosis is one of the most common causes of diarrhea globally. In 2015, a total of about 268,300 deaths occured from salmonellosis. In the United States, about 1.2 million cases and 450 deaths occur from nontyphoidal salmonellosis (one of the two common types) a year. In Europe, it is the second most common foodborne disease after campylobacteriosis. (A pair of Nile Monitors: As you can see, water is a big contaminant risk and major problem in Zoo maintenance.)
 Now called Deltaarterivirus hemfev, it is a highly pathogenic virus in monkeys Patas are believed to be the natural host for the virus since about 50% of wild patas monkeys have antibodies for the virus, while antibodies are much less prevalent in other simian species such as vervets and baboons. In macaques, however, infection with this virus can result in acute severe disease with high mortality. Recently, red colobus monkeys and red-tailed guenons have been identified as natural hosts for SHFV.
Now called Deltaarterivirus hemfev, it is a highly pathogenic virus in monkeys Patas are believed to be the natural host for the virus since about 50% of wild patas monkeys have antibodies for the virus, while antibodies are much less prevalent in other simian species such as vervets and baboons. In macaques, however, infection with this virus can result in acute severe disease with high mortality. Recently, red colobus monkeys and red-tailed guenons have been identified as natural hosts for SHFV.
I think its perfectly fine to call this Simian Fever, as I see it in many disease books referred to that way. Incidentally, some of our most dangerous diseases have jumped species from the monkeys. This usually requires blood or fluid contact though.
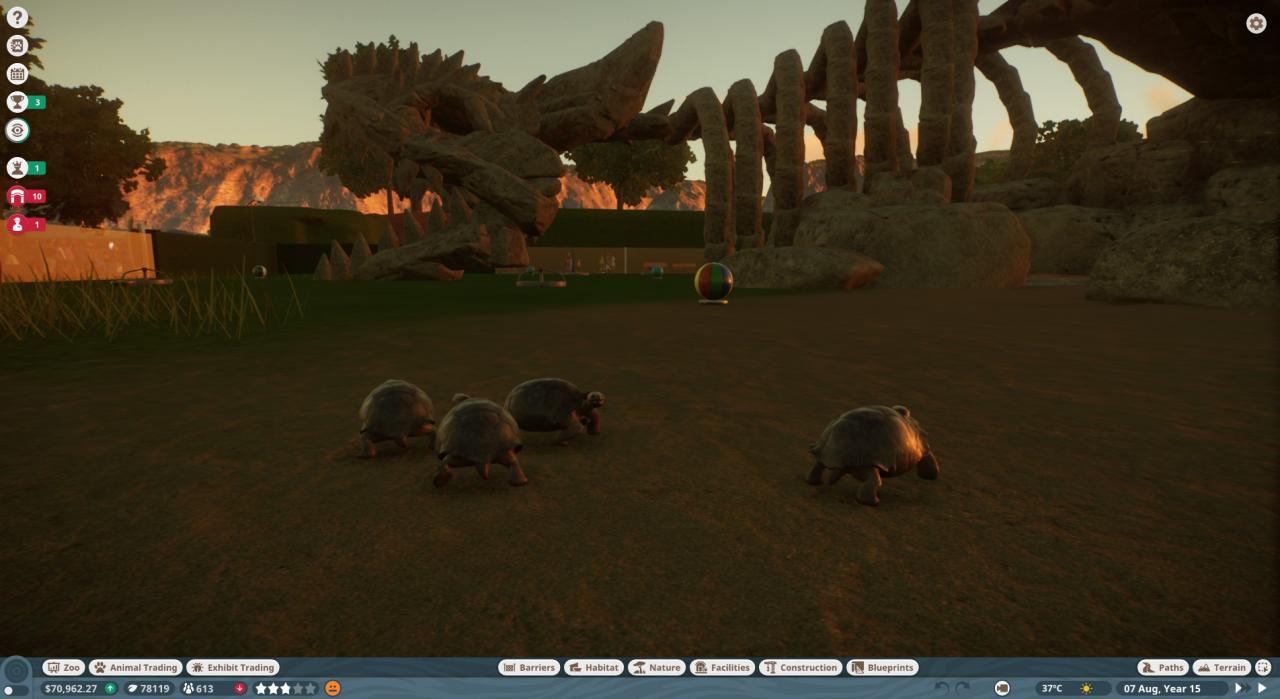 Testudinid herpesvirus 3 (TeHV-3) is the causative agent of a lethal disease affecting several endangered tortoise species. It is a disease that is still being researched to help us preserve tortoises in captivity and in the wild. I have found very little info about this disease and can pass on little.
Testudinid herpesvirus 3 (TeHV-3) is the causative agent of a lethal disease affecting several endangered tortoise species. It is a disease that is still being researched to help us preserve tortoises in captivity and in the wild. I have found very little info about this disease and can pass on little.(My screenshot shows the ‘Dragon Skeleton Cave Shelter’ workshop item in my Galapagos habitat. This is one of my favorite items by “Who are you people.”)
 Also known as lockjaw, tetanus is a bacterial infection characterized by muscle spasms. Tetanus is caused by an infection with the bacterium Clostridium tetani, which is commonly found in soil, saliva, dust, and manure.
Also known as lockjaw, tetanus is a bacterial infection characterized by muscle spasms. Tetanus is caused by an infection with the bacterium Clostridium tetani, which is commonly found in soil, saliva, dust, and manure.
Most non-zoo employed humans hear of tetanus when getting bit by an animal, and given a tetanus shot by the doctor.
 This is a bacteria spread disease which is also known as ‘rabbit fever.’ Symptoms may include fever, skin ulcers, and enlarged lymph nodes. Occasionally, a form that results in pneumonia or a throat infection may occur. The bacterium is typically spread by ticks, deer flies, or contact with infected animals. It may also be spread by drinking contaminated water or breathing in contaminated dust. It does not spread directly between people. (Fighting Gemsboks from my in-game screenshots.)
This is a bacteria spread disease which is also known as ‘rabbit fever.’ Symptoms may include fever, skin ulcers, and enlarged lymph nodes. Occasionally, a form that results in pneumonia or a throat infection may occur. The bacterium is typically spread by ticks, deer flies, or contact with infected animals. It may also be spread by drinking contaminated water or breathing in contaminated dust. It does not spread directly between people. (Fighting Gemsboks from my in-game screenshots.)
 Stomatitis is inflammation of the mouth and lips. It refers to any inflammatory process affecting the mucous membranes of the mouth and lips, with or without oral ulceration.
Stomatitis is inflammation of the mouth and lips. It refers to any inflammatory process affecting the mucous membranes of the mouth and lips, with or without oral ulceration.
In its widest meaning, stomatitis can have a multitude of different causes and appearances. Common causes include infections, nutritional deficiencies, allergic reactions, radiotherapy, and many others.It can appear in people and in a variety of animals, including house pets, and zoo animals.
Just as a random assumption, I would think that carnivorous predators would be at a greater risk for such medical issues. (Disclaimer: No bears were harmed in the making of this screenshot.)
 I noticed that the Giraffes seem safe at the moment. Are the devs racist towards aeronautic herbivores or something? Personally, I would like to experience the joy of keeping my lovely giraffes safe from Giraffe Skin Disease (GSD.) I feel so unneeded as it is in their habitat. They just graze around Zoorasia with no problems at all.
I noticed that the Giraffes seem safe at the moment. Are the devs racist towards aeronautic herbivores or something? Personally, I would like to experience the joy of keeping my lovely giraffes safe from Giraffe Skin Disease (GSD.) I feel so unneeded as it is in their habitat. They just graze around Zoorasia with no problems at all.
I am sure many Planet Zoo players have a disease or two in mind for inclusion in the game. Or, maybe you just want the game to show more of the visual signs of disease. Feel free to mention your ideas in the comments below, and I will add anything here that seems interesting.
While it is fun and convenient to mix species in some of your larger habitats, that is only a good option up to a point. As your number of animal bodies increases in a pen, you will need to subdivide the pen by species for two main reasons:
1. It just makes the Zookeepers’ job easier to feed them all.
2. It prevents the spread of disease among species.
The biggest safety for disease is to quarantine all animals when you buy them from the market, before placing them in your zoo. The vet will fix them right up and send them on their way to your beautiful habitats.
I hope you find some info here that is incredibly interesting. And, I am eagerly awaiting more animals to keep safe from these myriad diseases. Have fun!
Related Posts:
- Planet Zoo: How to Earn Massive Amounts of Conservation Credits
- Planet Zoo: How to Start a New Zoo
- Planet Zoo Animal List DLC Animals Included
- Planet Zoo: Beginner’s Guide to Franchise Mode
- Planet Zoo: Career Mode Guide
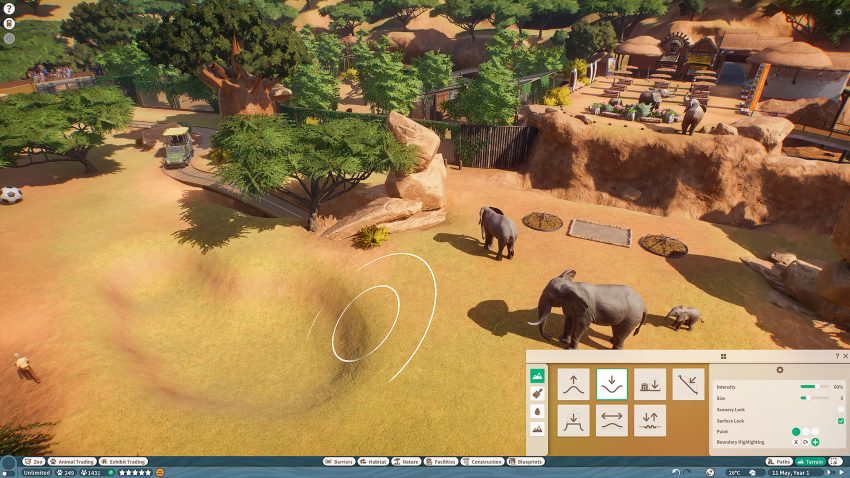
I was expecting aspergillosis ( fungal growth in respiratory tract due to the fungus Aspergillus) in the game, because it’s a common disease in captive animals especially birds. But I guess Frontiers world add it once they present ore bird species in future DLCs lol